Several years ago, I had an experience with my pug after giving her one of those hard, dehydrated, chicken strips for a snack. Almost immediately, she stopped breathing. I could see that she was fully obstructed, so I stood her up on her hind legs and attempted to perform the Heimlich maneuver. The first upward thrust didn’t clear her airway, so I tried it again (a bit harder) and out it came! A close call, for sure. Needless to say, I don’t recommend this type of snack as it poses a very high risk of choking.
But what could I have done if she had lost consciousness, or was pulled lifeless from a swimming pool? Is it possible to administer CPR for a dog or cat and how effective can it be?
Dr. Jamie Burkitt is an associate professor of Clinical Small Animal Emergency and Critical Care Service at the University of California, Davis. She also co-chairs an initiative spearheaded by a team of veterinary emergency and critical care specialists called The Recover Initiative. Not only does The Recover Initiative provide up-to-date evidence-based veterinary CPR guidelines, they offer affordable online classes to pet owners and pet professionals who want to learn these skills.
HOW TO KNOW IF YOUR DOG OR CAT NEEDS CPR?
According to Dr. Burkitt, pets, unlike humans whose heart’s may stop suddenly and without warning, will (most of the time) give some indication that they’re ill before their heart actually stops beating. Typically, these signs & symptoms include rapid or irregular breathing, lethargy, loss of appetite or excessive vomiting. If things continue to deteriorate and the animal becomes unresponsive you need to act.
Should this occur, do not call 9-1-1, begin CPR instead and have someone call the nearest veterinary hospital and let them know you are on your way. If someone else is driving you can continue to perform CPR on the way.
WHERE DO I DO CHEST COMPRESSIONS ON A DOG?
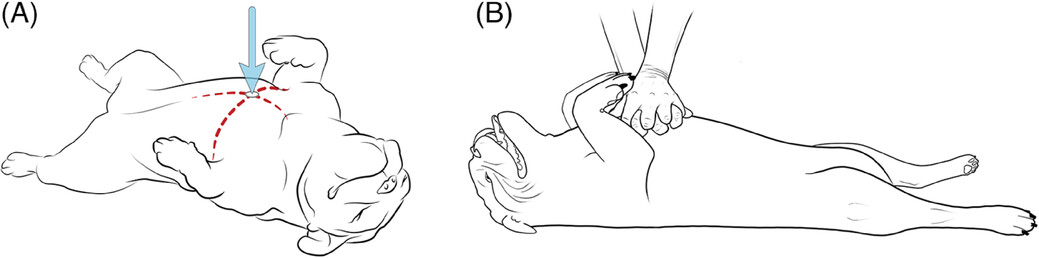
This varies depending on the size and breed of the dog. Chest compressions are typically done with the animal on their side but with dogs who have wider chests like an English Bulldog, for instance, it is better to do compressions while they’re on their back.
For round chested dogs such as retrievers, give compressions at the widest part of the chest. This should be done in the middle of their breastbone.
For medium and larger dogs, the rescuer should position themselves at the side, lock fingers together and keep your elbows locked, not bent, to achieve better quality compressions.
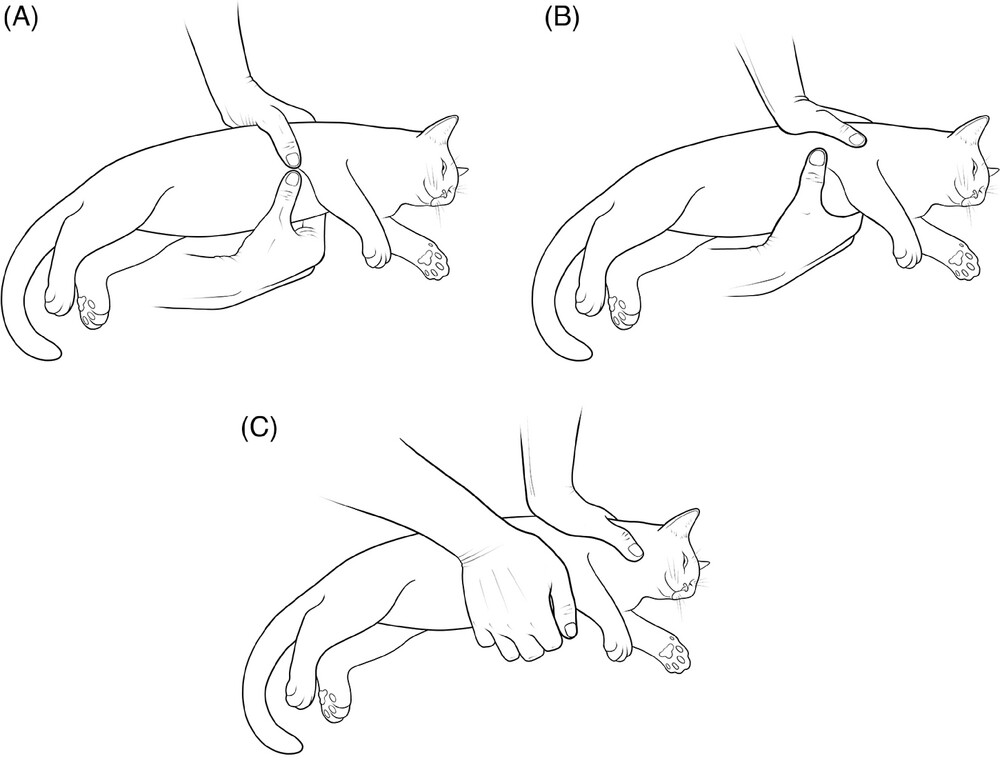
For smaller dogs or cats, use an overlapping, two handed compression method with your hands under their body and use your thumb(s) to provide the compressions.
Similar to human CPR the compression to rescue breathing ratio is 30 compressions: 2 breaths. Again, following the human format, the number of compressions per minute should be between 100-120 per minute. When delivering the rescue breaths encircle the nostrils of the animal with your lips to make a tight seal and blow hard enough to see or feel the chest rise.
Dr. Burkitt noted that there is little risk in administering CPR to a cat or dog and that the potential risk(s) are small compared to the need for life saving support.
Download a copy of the latest edition (2024) RECOVER CPR Guidelines here.
Information on The Recover Initiative Animal CPR and First Aid Course for Pet Owners and Pet Professionals is available here.
More information on CPR for Pets is available through The American Red Cross.